Many children growing up in Bangkok are bilingual, meaning they are exposed to more than one language. This post addresses some common questions and misconceptions about bilingualism, to further guide parents and educators about this topic. What does Bilingual mean? Bilingualism can look like many different things. Below are some examples:
Does Bilingualism cause language delay? No, learning two languages simultaneously does not cause confusion or language delay (1). In fact, in contrast to this common misconception, only speaking English to your child when it is not the parents’ native language can make it harder for the child to learn any language well, as the quality and quantity of language exposure is limited. This means that multilingual families should speak to their child in the language in which they feel the most comfortable and fluent in. Is it a Language Disorder? Or Language Difference? Language Disorder refers to difficulty in learning, understanding and expressing in any language. This means the child shows delay or atypical language development compared to the expected level of their age, even in their mother tongue or first language. Language Difference is when a child is developing as typically expected in their native language, however, they are having difficulties learning a second language. For example, difficulty with English used for instructions at school or with the language used by the greater population in the area where they live. Does my child need Speech Therapy? If you suspect language delay in your bilingual child, the first step is to consult with a Speech Language Therapist, who can conduct a Speech Language Evaluation, ideally in your child’s first language. Bilingual Speech Therapists can deliver therapy in your child’s native language, which can promote development in both languages. This article was written by guest writer, Siu Wai Wong (Mr. Leon), a bilingual Speech Language Pathologist. He has also translated the article into Traditional Chinese and Simplified Chinese languages below. Speak soon, The Expat Speechie Reference: 1. Paradis, J., Genesee, F., & Crago, M. (2011). Dual Language Development and Disorders: A handbook on bilingualism & second language learning. Baltimore, MD: Paul H. Brookes Publishing. --- 中英文雙語言語治療 許多在曼谷長大,或在泰國接受教育的小朋友都會接觸到多種語言,我們稱他們為雙語兒童。以言語治療師的觀點,以下將探討家長和教育工作者對於雙語兒童常見的疑問。 什麼是「雙語兒童」?
會因為學雙語而「造成語言障礙」嗎? 根據目前各種研究顯示:當孩子同時學習兩種語言以上時,並不會有直接的負面影響。但家長要留意,倘若家長對英語的掌握只是一般的水平,孩子從家長身上模仿也只是簡單表面的詞彙、句子結構,未能達到靈活運用的效果,反之,孩子接觸及練習母語的機會亦相對減低,因而影響母語的學習進度。只要父母或照顧者使用自己本身最舒服並且擅長的語言,孩子都能夠自然而然地吸收進而運用。 區分「語言障礙」和「語言差異」
我的子女需要接受言語治療嗎? 如果您的雙語子女在語言方面有明顯且持續的困難,請安排與雙語言語治療師使用孩子母語或雙語進行發音和語言評估。治療師會根據評估結果診斷孩子是否語言發展遲緩,提供相對的雙語訓練與治療。 引用: 1. http://scrc.com.tw/?p=1813 --- 中英文双语言治疗 很多在曼谷长大,或在泰国接受教育的小朋友都会接触到多过一种语言,我们称他们为双语儿童。以语言治疗师的观点,以下将探讨家长和教育工作者对于双语儿童常见的疑问。 什么是「双语儿童」?
会因为学双语而「造成语言障碍」吗? 根据目前各种研究显示:当孩子同时学习两种语言以上时,并不会有直接的负面影响。但家长要留意,倘若家长对英语的掌握只是一般的水平,孩子从家长身上模仿也只是简单表面的词汇、句子结构,未能达到灵活运用的效果,反之,孩子接触及练习母语的机会亦相对减低,因而影响母语的学习进度。只要父母或照顾者使用自己本身最舒服并且擅长的语言,孩子都能够自然而然地吸收进而运用。 区分「语言障碍」和「语言差异」
我的子女需要接受语言治疗吗? 如果您的双语子女在语言方面有明显且持续的困难,请安排与双语语言治疗师使用孩子母语或双语进行发音和语言评估。治疗师会根据评估结果诊断孩子是否语言发展迟缓,提供相对的双语训练与治疗。 引用:1. https://m.ourbethel.cn/lists/details/pid/1/id/646c5bf4b679782805b85c4c One of the common concerns which parents express about their child's early development has to do with their eating. This may include their child refusing to eat, not eating enough or being a 'picky eater'. It is important to address these concerns as they directly impact a child's nutrition, growth and development.
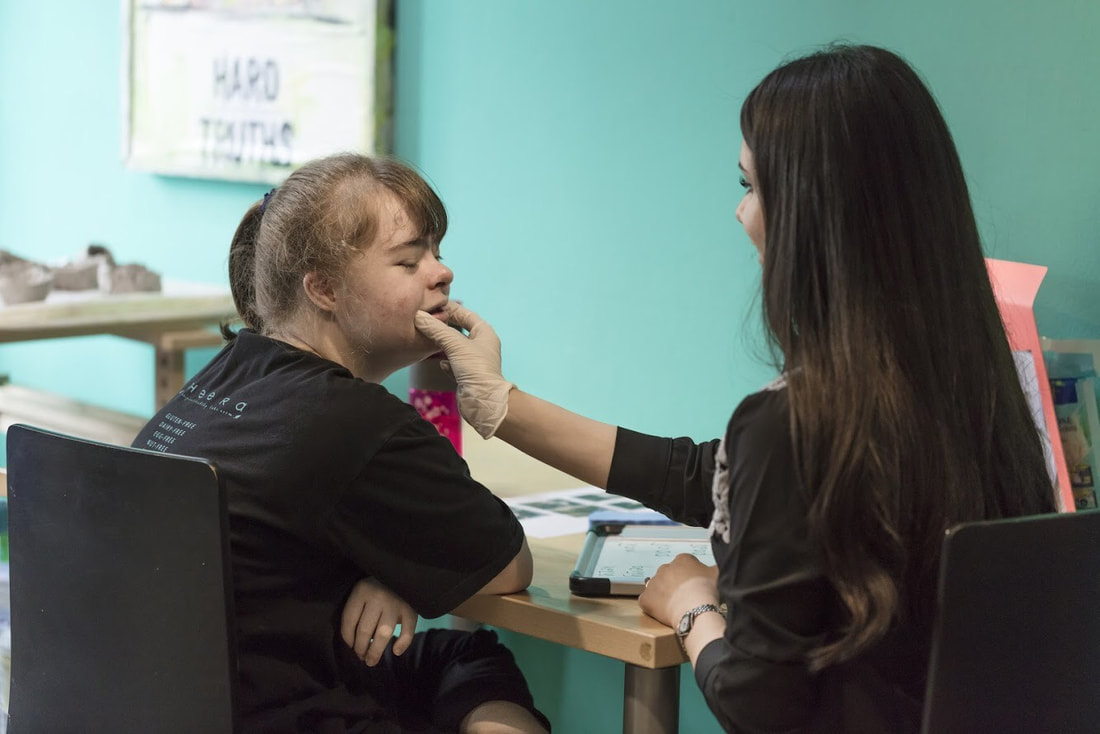
This is where the SOS Feeding Approach comes in! SOS stands for Sequential Oral Sensory, an evidence based, multidisciplinary, multi-system approach developed by Dr. Kay Toomey that addresses feeding issues in children. The main objective of this approach is to prepare and support the children in learning the skills required to eat. Picky eater or Problem feeder? Some children go through a stage of refusing certain foods, some others have oral motor or sensory issues that contribute to challenges with eating. Some signs that feeding is a problem include: ● Having a limited range of foods, usually less than 20 foods ● Weight and height are lagging on growth chart ● Coughs or gags during mealtimes, or have reflux issues ● Refusing to eat food they once ate regularly ● Refusing entire food groups such as vegetables or textures such as solids ● Responding emotionally when presented with new food, such as by crying or walking away Does my child need Feeding Therapy? If you are not sure if your child needs Feeding Therapy, they may benefit from an initial Feeding Screening with S.O.S trained Therapist to evaluate their eating skills or feeding issues. The therapist can provide a personalized play-based treatment program which focuses on food to support your child in developing the skills and tolerance to progress through ‘Steps to Eating’ (listed below). The aim of this program is for your child to learn how to eat a wider variety and range of foods, to meet their nutritional needs and support their growth and wellbeing. 6 Steps to Eating: Step 1: Child tolerates the food Step 2: Child interacts with food Step 3: Child smells the food Step 4: Child touches the food Step 5: Child tastes the food Step 6: Child eats the food It is important to be mindful that eating a range of foods doesn't happen right away. Children often need to be exposed to and comfortable with food textures, smells and tastes as the initial steps. Also, it is encouraged to have a little fun and mess along the way! This article was written by guest writer, Siu Wai Wong (Mr. Leon), a bilingual Speech Language Pathologist. He has also translated the article into Traditional Chinese and Simplified Chinese languages below. Speak soon, The Expat Speechie --- 解決孩子進食問題: S.O.S 進食治療法 很多家長都有經歷過正餐時候,小朋友沒有食慾、不肯進食或者不願自己進食等的情況。到底如何幫助兒女解決飲食方面的問題呢?或許以下介紹的S.O.S進食療法會適合您的孩子。 SOS進食療法是一個有科學依據的系統性進食療法。這種方法同時強調感統和口腔肌肉在進食過程中的重要性,幫助孩子克服進食方面的障礙。 挑食 VS 進食困難? 有些孩子會在成長過程中經歷挑食的階段,僅吃幾種自己喜歡或習慣的食物,但有些有進食困難的孩子,他們的口肌或感統問題會引致以下表現:
我的子女需要進食治療嗎? 如果您擔心您孩子的飲食,請與接受過S.O.S訓練的治療師諮詢並為您的子女進行進食評估,從而提供診斷和治療方案。進食治療過程融合以食物為主的遊戲,促進孩子進食能力,如咀嚼技巧和提升他們對多種食物的接受程度,以助他們攝取足夠的營養,滿足成長所需。 學習進食不同種類和質感的食物需要時間。在治療師和家長的幫助下,小朋友可以開始學會接受和接觸更多的食物,在遊戲和感官學習的過程中逐步為他們的餐單添上色彩! --- 解决孩子进食问题: S.O.S 进食治疗法 很多家长都有经历过正餐时候,小朋友没有食欲、不肯进食或者不愿自己进食等的情况。到底如何帮助儿女解决饮食方面的问题呢?或许以下介绍的S.O.S进食疗法会适合您的孩子。 SOS进食疗法是一个有科学依据的系统性进食疗法。这种方法同时强调感统和口腔肌肉在进食过程中的重要性,帮助孩子克服进食方面的障碍。 挑食 VS 进食困难? 有些孩子会在成长过程中经历挑食的阶段,仅吃几种自己喜欢或习惯的食物,但有些有进食困难的孩子,他们的口肌或感统问题会引致以下表现:
我的子女需要进食治疗吗? 如果您担心您孩子的饮食,请与接受过S.O.S训练的治疗师咨询并为您的子女进行进食评估,从而提供诊断和治疗方案。进食治疗过程融合以食物为主的游戏,促进孩子进食能力,如咀嚼技巧和提升他们对多种食物的接受程度,以助他们摄取足够的营养,满足成长所需。 学习进食不同种类和质感的食物需要时间。在治疗师和家长的帮助下,小朋友可以开始学会接受和接触更多的食物,在游戏和感官学习的过程中逐步为他们的餐单添上色彩! Parents often ask, "does my child have a voice disorder?" Below are some questions which can be used as a guide to know whether or not your child's voice is something to be concerned about.
1. Does your child's voice draw attention to itself, to the extent that it distracts listeners from what your child is actually saying? 2. Does your child's voice briefly disappear at times, or disappear for long periods? 3. Does your child's voice limit them when they are participating in daily activities? 4. Does your child's voice sound strained and effortful? If the answer to any of these questions above is 'yes', it is recommended that your child's voice is assessed by a Speech Therapist. In the meantime, below are 8 things that you can encourage your child to do, to protect their voice.
Also, here are 3 things you can do, to further protect your child's voice.
Finally, if you think that your child's ongoing voice problems may have a structural cause, a consultation with an Ear Nose and Throat (ENT) Specialist can confirm or rule this out. Speak Soon, The Expat Speechie Learning to express emotions is such an important life skill. Often, tantrums and meltdowns happen because a child cannot yet express how they feel in a situation. Giving your child the tools to express their emotions will improve their communication skills, empower them to express themselves and ask for help, as well as reduce tantrums and meltdowns.
Here are 7 simple tips for teaching your child to use emotion words. 1. Tell your child what you see You may notice that your child has a meltdown or tantrum when they do not have the words, or do not know how to express what they are feeling. Giving your child these emotion words is a powerful tool to help them feel understood in a situation where their emotions are building up. For example, if your child is upset that they cannot have their way about something, you can put this into words for your child by saying, “I can see that you are frustrated”. 2. Play mirror games Pick an emotion and make a face in the mirror which shows this emotion. Ask your child to look in the mirror and imitate the face you have made. Then write the emotion word this face depicts on the mirror with a mirror crayon. To make it even more fun, ask other family members to join in. 3. Take photos Emotions have long been taught through drawings of stick figures and facial expressions. However, for a lot of our children, these drawings are too ambiguous and often hard to interpret. Instead of these drawings, take photos of yourself, or someone else in your family making faces that depict different emotions, or ask your child to imitate you making faces that show different emotions. Print these photos and label the emotion under them. You can then hang these photos on a picture board or on a line with pegs in your child’s room as a visual reminder. 4. Draw attention to how the emotion feels A great way to teach your child emotions is to talk about how they make the body feel. For example, bring your child’s attention to how angry makes your face feel hot, your hands and teeth become tightly clenched, your heart beats faster. Also, ask your child to describe how different emotions make them feel. Use a drawing of a shape of a person as a visual cue to get the conversation going. Your child can then circle body parts on this drawing and talk about how they feel. 5. Incorporate stories A powerful way to teach your child about emotions is to tell them a story. A story will bring context to the learning, to help your child understand the emotion in a specific situation. The story will have even more of an impact if it is based on real people and includes photos of these people, including your child. Your child will likely remember this story for a long time. 6. Use Self-regulation Tools A fantastic self-regulation tool which I use with children who I work with are the 'Zones of Regulation'. This tool is based on the idea that there are 4 colour zones which your child can be in (red, yellow, blue and green), and each zone is associated with certain emotions. Your child will learn to associate the emotions with certain colour zones. For example, your child may eventually express that they are in the "blue zone" when they are feeling sad, or the "yellow zone" when they are feeling nervous or excited. Then, your child will learn about different strategies / tools which they can use in each colour zone. For example, counting to 10 or drawing to get into the 'green zone'. You can read more information about the Zones of Regulation here. 7. Reassure that it is OK to feel emotions When teaching your child about emotions, it is important to tell them that it is OK to feel all the emotions. For example, I often tell my students, "it is ok to feel frustrated. Everyone feels frustrated sometimes". Also, try to avoid placing judgement on emotions (e.g. feeling angry is 'bad'). Doing these 2 things, will allow your child to express themselves without feeling like what they are experiencing is out of the ordinary, and will let them know that you can relate to what they are feeling. Speak soon, The Expat Speechie  Staying home means more opportunities for conversations with your child. The good news is, you don’t need to be an expert on conversation starters with your child! Below are 5 tips to maximize your conversations together.
2. Cut back on the questions To have great conversations with your child, reduce the number of questions you ask them. Try to avoid questions that ‘test’ or ‘check your child’s knowledge on a topic, an area, or a word. Instead, ask questions that show your interest in the topic you are speaking about, and that your child will enjoy responding to and telling you about. 3. Tell your child a short story Research shows that when people hear a story, certain brain areas are activated, which make people experience being in that situation. As a result of this, we remember stories more than facts. So, try to tell your child a story. Your child will enjoy the experience more than if you were telling them a fact, and it is likely that your child will remember this story later in their life. 4. Listen more The same principles apply here to having a conversation with an adult - listening makes you a better conversation partner. So, in your next conversation with your child, try to take a step back by saying less, waiting, and showing that you are listening. Also, remember those non-verbal cues of looking at your child, and avoiding distractions in the home or looking at your phone during the conversation. Your child will likely want to tell you more in response to this. 5. Model correct conversational communication You are your child’s main language model, and conversations are a strong tool for stimulating your child's speech and language. In your next conversation, be sure to use an adult-like tone of voice, speak in complete sentences with correct grammar, and introduce a new word every now and then (try not to over do it with the frequency of new words). This will give your child a correct speech and language model during your conversations together. Speak soon, The Expat Speechie  With the recent closure of all schools and child development Centres across Thailand, hundreds of children now do not have access to in-person Speech Therapy. While this closure period has been predicted to last a total of 5 weeks in Thailand, there is a possibility that it might go on for longer, without a predictable end-date in sight. So, does this mean that children who were attending regular Speech Therapy can not have Speech Therapy for as long as this closure period lasts? Absolutely not! Especially if there is an openness to other forms of Therapy, beyond the ‘traditional in-person Therapy model’, where the therapist and child are together in the same room. In fact, there is an increasingly popular solution to overcome these barriers, called 'Teletherapy'. Let me tell you more about Teletherapy, below. What is Teletherapy? Teletherapy involves the use of communicative technology to provide Speech Therapy services, such as video-conferencing, email, and telephone. Nowadays, Zoom and Google Meet are popular online platforms for Teletherapy sessions. What do parents think? It is understandable that some parents are more comfortable with traditional in-person therapy, as they are more familiar with this. However, these days, in-person Therapy is not an option. Undoubtedly, a newer form of Therapy is better for every child’s development, than no Therapy. The common misconception is that Teletherapy will not be as effective as traditional therapy. However, scientific research has proven that this is not the case. What does the research say? Teletherapy has been widely used to assess, diagnose, provide treatment and support to children and their families [1]. Scientific research has shown that Teletherapy results in similar outcomes for both diagnosis and treatment when compared to traditional in-person therapy [2]. Teletherapy can also be a sustainable solution on a wider scale, such as, when used in schools where many children attend Speech Therapy weekly. An Australian study investigated the effectiveness of Teletherapy in school settings [3]. The findings of this study showed that most of the goals outlined for the children receiving Teletherapy at school were achieved at the level expected, or beyond [3]. Why Teletherapy? Here are some benefits of Teletherapy: 1. It is the safest option for your child and family at the moment Since Teletherapy does not involve direct contact between people, there is no risk of spreading germs or a communicable disease during the online session. 2. Teletherapy practice is context-relevant During traditional in-person Therapy, children typically practice skills in a Therapy setting, such as the clinic, or in a 'speech room' at school. Children are then expected to transfer these skills in their natural environment, at home. However, Teletherapy removes the entire pre-transfer practice layer and gets straight into practice in the home environment. Practicing skills at home allows children to make the association between these skills and their home environment - this is likely to support children to apply these skills during daily interactions at home. 3. Flexible consultation time Teletherapy allows for more opportunities for consultation times than traditional in-person sessions, for both parents and therapists. 4. Eliminates travel time Children and parents can become exhausted after traveling long-distances- or being stuck in traffic over short distances, such as in Bangkok. Similarly, therapists also become tired when traveling long distances, which may impact on the frequency of the visits arranged [5]. Personally, I have been stuck in traffic for time periods longer than the total Therapy time scheduled at a school or Centre before! Teletherapy eliminates this need for parents, children, and therapists to travel for sessions. 5. Wide applicability Teletherapy is being used in the assessment and treatment of many areas of speech and language delays and communication disorders [3]. These include articulation, Autism, cognitive-communication disorders such as after traumatic brain injury, language delay, stuttering, voice disorders, and swallowing difficulties. 6. Gives you a break! Teletherapy allows you to take a break, while your child is engaged in active learning online with their therapist. Your child's therapist can then update you about the session and provide homework for your child to practice throughout the week. Teletherapy is an accessible, safe, effective, and time-efficient way to have Speech Therapy. Most importantly, the outcomes of Teletherapy have been proven similar to those of traditional in-person therapy. I hope that more people will consider this option for their child during this school closure period, and beyond. Speak soon, The Expat Speechie References Acknowledgement and thanks to the following sources whereby the above information was obtained: [1] Reynolds, A. L., Vick, J., & Haak, N. J. (2009). Tele-health applications in speech-language pathology: Journal of Telemedicine and Telecare, 15, 310-316. [2] Edwards, M., Stredler-Brown, A., & Todd, K. (2012). Expanding use of tele-practice in speech-language pathology and audiology. The Volta Review, 112, 227. [3] Fearweather, C., Lincoln, M., & Ramsden, R. (2016). Speech-language pathology teletherapy in rural and remote educational settings: Decreasing service inequities. International Journal of Speech-Language Pathology, 18, 592-602. [4] Anderson, K. L., Balandin, S., & Stancliffe, R. J. (2015). Alternative service delivery models for families with a new speech-generating device: Perspectives for parents and therapist. International Journal of Speech Language Pathology, 17, 185-195. [5] Dew, A., Vietch, C., Lincoln, M., Brentnall, J., Bulkeley, K., Gallego, G., et al. (2012). The need for new models for delivery of therapy interventions to people with a disability in rural and remote areas of Australia. Journal of Developmental Disability, 37, 50-53. This month's post is written by guest writer, Camila Gutiérrez, a fabulous Occupational Therapist (Sensory-Motor Development Specialist), who is living and working in Bangkok. I hope you find the recommendations in this post informative and practical during your family's time indoors.
Speak soon, The Expat Speechie --- Following developments of Covid19 in Bangkok, all schools in Thailand are now closed and social distancing is being strongly encouraged. But what do all these sudden changes really mean for our children? - Closed school will change your child’s daily routine, involving less structure, social participation, and interaction with peers. Your child might be thinking, ‘What happened to my routine?’ - Since you are avoiding crowded places, such as going to the cinema or playing outside, your child might be thinking, ‘I am not playing with my friends’. - Self-quarantine at home means increased leisure time at home, which does not necessarily provide your child with the sensory opportunities they need. Your child might be thinking, ‘I usually have playtime outside at school - where can I run, climb, and jump in here?’ During this period, you can expect to see more unwanted behaviors because of all the changes. It is important to remember, that underneath these behaviours, what your child is trying to communicate is, "I need movement!" With some simple strategies, your child will learn to adapt, and you can provide them with the movement and sensory stimulus they might be seeking while at home. 1. Try to remain calm, even if your child is showing some changes in their behaviour. Your child will see that you are calm, which sends them a message that there is no reason to be alarmed. 2. Take data to understand your child’s new behaviours. If you see that your child is having tantrums or meltdowns, the first step is to identify what is triggering this. A simple way to address this is by taking “ABC” (antecedent – behaviour – consequences) data. Sometimes we just focus on the behaviour, but it is just as important to look into what happened before the new behaviour (e.g. was there some change? Did something go wrong? was there a sensory overload?, etc). It is also important to look at what happened after the behaviour (e.g. why this behaviour is continuing? did we act reinforcing the behaviour? etc.). 3. If your child will attend online classes, schedule some movement breaks. These are breaks for 5 to 10 minutes between tasks that allow children to move. Movement breaks improve attention, allow your child to integrate information, as well as to regulate their emotions. Movement breaks can include:
4. Try to establish a new productive routine: As you know, children need to be occupied by different things throughout the day. Try to establish structure by creating a new routine that includes sleep, self-care, leisure, and productivity. That will help to create habits, roles, and to increase their independence. Your child can also help with responsibilities at home such as, making their bed, cleaning the room, help to prepare during mealtimes, etc. 5. Incorporate a Sensory Diet throughout the day. A Sensory Diet is a group of activities that are specifically scheduled into a child’s day to meet their sensory needs. Sensory Diets include specific types of input, such as proprioceptive (e.g. pulling, pushing, carrying heavy items), tactile (e.g. playdough, soft blankets), visual (e.g.marching games, calm down bottle), auditory (e.g. listening to music), vestibular (e.g. somersaults, hanging or lying upside down), gustatory (e.g. strong flavor snacks), and oral motor (e.g. blowing bubbles, eating crunchy snacks, drinking from a straw). Sensory diets support your child’s brain to regulate attention and maintain an appropriate level of arousal. It is important to include both alerting and calming activities in your child’s Sensory Diet. Below, are examples of both types of activities. Some alerting activities for your child can include:Hang upside down Hang on a bar Jump on the couch/bed Crawl Tung on a rope Jumping jacks Jump-rope Wheelbarrow walk Jump and fall on pillows Some calming activities for your child can include:Warm bath Soft music Receive a massage Squeeze Hug Hold a vibration toy Put on lotion Smell essential oils Look at calming bottles You can also create an obstacle course. You can use blankets, chairs, pillows, balloons, bubbles, puzzles, slime, balls. Make sure this includes:
6. Include board games during the day. Board games are beneficial for your child to practice their language, communication, and social skills. By playing board games, your child will practice teamwork, turn-taking, achieving a goal, problem-solving, being a good winner, but most importantly, being a good loser. If you are a parent who wants to know more about supporting your child’s sensory needs while indoors, you can contact me at camila@littlesproutscentre.com. I am also offering Skype coaching and/or parents consultation to new families during this period. Stay safe! Camila Gutiérrez, OTRL Occupational Therapist  If you have noticed that your child’s tongue constantly pushes through their front teeth at rest, while eating, or speaking, your child may have what is called a ‘tongue thrust’. This is a behavior pattern which is sometimes referred to as an “immature swallow”. Many children will outgrow this by themselves. But if this is not outgrown by a young age, this habit is likely to strengthen, and will become harder to correct as they get older. There are steps that can be taken to address and correct your child’s tongue thrust. This month’s post brings you a step-by-step action plan to do so. Step 1: Monitor The first step is to monitor your child and collect patterns over a time period. Below are some questions to guide your monitoring process:
Step 2: Physical Examination The next step is to arrange a consultation with an Ear Nose and Throat Specialist (ENT). This is such an important step because it addresses the underlying cause. The observations you made when monitoring your child (above) will play a big role in this step, so be sure to discuss them with the ENT. An ENT is specialized to observe, confirm or rule-out any structural / physical conditions which might be causing this. For example, your child’s tonsils may be enlarged, or your child may have chronic allergies. Both of these will lead to mouth breathing, and your child’s tongue to protrude outside of their mouth. Mouth breathing is critical to address because it can impact your child’s sleep, the structure of how their face forms, their alertness, overall comfort level, their eating, their behavior and their mood. Step 3: Address Structural / Physical Factors This step is different for all children; it will depend on what the ENT finds and recommends. For example, this may involve an operation to remove your child’s tonsils, or medicine to manage their chronic allergies. This step will help your child to breathe through their nose, which will physically allow them to then work on a closed-mouth posture. Step 4: Consult with a Therapist Addressing tongue placement for habit, breathing and eating Sometimes, it may not be a structural or physical cause. Instead, the reason why your child’s tongue may be outside of their mouth constantly could simply be a habit. Myofunctional Therapists or Oral Placement Therapists are most specialized in addressing these habits, and correcting tongue placement in the mouth with a range of exercises. Speech Therapists who are specifically trained in Oral Placement Therapy, can also work with your child to correct their tongue placement at rest, for breathing, and for eating. Addressing tongue placement for speech If your child has a tongue thrust, they likely have a lisp on certain sounds, such as ‘s’ and ‘z’. All Speech Therapists are specialized to work with your child to correct their tongue placement in speech sounds. The Therapist you consult with will develop an Intervention plan that best suits your child’s needs, and may also provide exercises for home practice. Step 5: Dentist Constant tongue protrusion outside the mouth will eventually push your child’s teeth outwards. If it is age-appropriate, and if you would like to have a Dentist realign your child’s teeth, it is recommended that you do so after your child has attended several Therapy sessions (step 4 above). This will avoid your child’s teeth continuing to be pushed outwards after they have been realigned. Speak soon, The Expat Speechie  Did you know that your child has 7 senses? Most people think that children only have 5 senses - touch, sight, sound, smell and taste. However, your child (and you) have 2 additional, or ‘hidden’ sensory systems, that work together to organize and regulate the other senses. These 2 hidden sensory systems are the proprioception sense, which gives your child information about body position and the movement of their body parts, and the vestibular sense gives your child information about the position of their head in space and their balance. Your child’s 7 senses all work together to achieve ‘sensory integration’. Sensory integration is how your child uses the information from their body and the environment to respond to daily challenges and new circumstances (emotional, social or cognitive learning). Sensory Integration helps your child with their self-regulation, self-care, activity level, attention, social functioning and emotional regulation. However, most children with special needs find it hard to understand the sensory information from their bodies and their environment. This is called Sensory Processing Disorder. If your child has Sensory Processing Disorder, you might notice that:
There are ongoing challenges for children with Sensory Processing Disorder, which can interfere with their daily life and with learning. If your child’s senses are not regulated, it is difficult for learning to happen in any environment, including in class or during a Therapy session. For example, it would be difficult for your child to focus on learning new vocabulary and social skills if they need to move constantly without the ability to sustain their attention and engagement. Another example is, it would not be possible for a Speech Therapist to give your child tactile cues for speech sounds by touching their face, if they are over-responsive to touch. However, your child can still learn many skills while having a Sensory Processing Disorder. The key is to create the right conditions for learning before the teaching happens. A great way to achieve this is combined Speech Therapy and Occupational Therapy sessions. Instead of your child working on skills in isolation, these combined sessions focus on your child’s learning, while meeting their sensory needs. During these sessions, the Occupational Therapist will first regulate your child’s senses to create the optimal conditions for learning and provide the sensory inputs required for your child to be alert and attentive. The Speech Therapist will then engage your child in learning and teach them the skills necessary to improve their communication. From our experience working with children abroad and in Thailand, children respond well to these combined Speech and Occupational Therapy sessions and learning tends to happen quickly. We hope to see more of these combined sessions in Thailand in the years to come. This article was written by: Chiman Estephan, MSLP, MSPA, CPSP, ACAS Advanced Certified Autism Specialist & Speech Language Therapist Camila Gutiérrez V, OTRL Occupational Therapist (Sensory Integration Specialty) Speak soon, The Expat Speechie Thinking skills are such an important part of your child’s development. Good thinking skills can help your child make good choices, come up with creative ideas and try to solve their problems independently.
Here are 10 simple techniques you can use throughout the day to stimulate your child’s thinking skills: 1. Schedule ‘free-time’: This may seem counter-intuitive. Children growing up in Bangkok usually go from school to a series of after-school lessons. While this stimulates a child’s learning and gives them new skills, it is important to realize that this is all structured time with little opportunities to think independently. So, try to leave a daily time open in your child’s schedule for unstructured ‘free time’. 2. Pretend-play: Play serves as an important foundation for thinking and language. When your child pretends during play, they learn to associate a toy, or a pretend-event, with a real object or a real event. Pretend-play helps your child think about the world around them and understand it better. 3. Limit and rotate toys: Good news – there is no need to constantly buy new toys. No matter how many toys you buy, your child will eventually become bored of all of them. Instead, keep toys the same and rotate the toys, every few days. Encourage your child to use these same toys to create new situations or to use them in new ways. For example, your child can use a toy-rock as a phone during play, or use a sheet of paper as a blanket. This is called substitution-play and it is great for expanding your child’s thinking through their imagination. 4. Familiar stories with new endings: More good news – you also do not have to keep buying new books. Yes, your child might become familiar with the stories that you read to them, or that they have started reading by themselves. But, you can keep these books interesting by stopping half-way or towards the end and asking your child, “how do you want the story to end this time? Why do you want this to happen?” This will make your child think more than if they are simply listening to a story. 5. Stop and Wait: When your child has a question or a small problem, it is intuitive to immediately step-in and help. Instead, try to stop and wait first. This will give your child the chance to think for themselves and attempt to solve their problem creatively or independently. By assuming competence, you empower your child to think independently. 6. Teach reasons, as well as rules: During speech therapy sessions, I usually explain the reason behind each rule I give. I have found that this helps children understand the purpose of rules, which makes them more likely to follow the rules. So, the next time you give your child a rule, try to explain the reason why this rule exists. You might be surprised at how they respond once you expand their thinking and understanding this way. 7. Ask open-ended questions: Questions like ‘why’, ‘how’ and ‘what if’ will help your child to expand their thinking and creativity. One way you can do this is after watching a movie together. For example, “why do you think this happened in the movie?” Another way you can do this is when your child asks you for something, “why do you want a new bike?” 8. Think out loud: You can model thinking to your child by thinking out loud. You can do this throughout the day during your routines or when you make a decision. For example, before leaving home together, “look at the clouds in the sky, it’s going to rain today. I think we should take the umbrella”. 9. Teach a second language: Research studies have shown that being bilingual has many cognitive benefits, including improved memory, ability to learn new things and flexibility between tasks. Interestingly, there is research showing that the cognitive benefits of being bilingual start from the young age of 7-months (Kovacs & Mehler, 2009) . 10. Finally, encourage your child to ‘explore’ their surroundings outside. After all, thinking and creativity is limited between four walls! Speak soon, The Expat Speechie Reference: Kovacs, A., & Mehler, J. (2009). Cognitive Gains in 7-month old Bilingual Infants. PNAS, 106, 6556–6560. |
Welcome to my blog!
|